(CN) – Florida officials declared a public health emergency over the rapid spread of Hepatitis A across the Sunshine State, as thousands of vaccines are being handed out for free each week.
 Over 2,000 people have come down with the communicable disease this year, according to records kept by the Florida Department of Health. By contrast, Florida reported 548 Hepatitis A cases for all of 2018.
Over 2,000 people have come down with the communicable disease this year, according to records kept by the Florida Department of Health. By contrast, Florida reported 548 Hepatitis A cases for all of 2018.
Twenty-eight people have died after contracting the vaccine-preventable disease, which attacks the liver, since early 2018.
"I am declaring this public health emergency as a proactive step to appropriately alert the public to this serious illness and prevent further spread of Hepatitis A in our state," Florida Surgeon General Dr. Scott Rivkees said in a statement Thursday.
The declaration will allow the Centers for Disease Control and Prevention to assist the state in controlling the outbreak.
“With Florida being the third largest state in the country, it is unfortunate, but not surprising that our case numbers have also been rising,” Dr. Carina Blackmore, the state epidemiologist, said at a recent press conference.
The majority of reported cases in Florida are concentrated in the Tampa Bay area.
"I wouldn’t have a definite answer as to why we have the highest number of cases," Pinellas County Department of Health spokesperson Maggie Hall said in an email. "I wish all of us knew that."
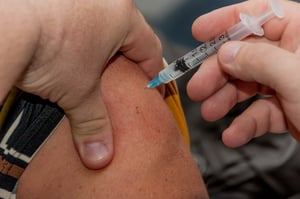
In order to slow the spread of the disease, county health officials are sending out roving units of nurses armed with the vaccine. The health workers visit restaurants to inoculate workers and stroll through parks to immunize the homeless. All Florida counties are offering the vaccine for free. The Department of Health estimates 5,000 vaccines are distributed each week across the state.
The Hepatitis A virus spreads through the feces of infected people. Individuals who do not wash their hands after using the bathroom can transfer the virus via food, drinks or drugs. The virus can live outside the human body for months.
The virus attacks the liver and can lead to serious complications in at-risk people. Some people may not feel anything for two weeks before fever, fatigue, nausea, vomiting and abdominal pain set in. The symptoms can worsen with joint pain and jaundice, and can last months.
Although the public tends to focus on reports of restaurant workers who test positive, the CDC says most cases come from homeless individuals and drug users.
As a whole, the United States has experienced a recent increase in Hepatitis A cases after years of decline. Since the first vaccine became available in 1996, the CDC estimates Hepatitis A rates decreased by 95% until 2017, when outbreaks appeared in more than a dozen states.
Kentucky, hit hard by the opioid crisis, has the most reported cases of Hepatitis A in the country.
Subscribe to Closing Arguments
Sign up for new weekly newsletter Closing Arguments to get the latest about ongoing trials, major litigation and hot cases and rulings in courthouses around the U.S. and the world.








