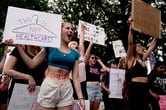SAN FRANCISCO (CN) — Counsel for a class of more than 3 million Californians urged jurors to use common sense in deciding whether Northern California’s largest hospital chain kept healthcare costs high by forcing health insurers to accept onerous contract terms, as a landmark antitrust trial against Sutter Health came to a close Wednesday.
“Sutter knowingly harmed premium payers for its own selfish purposes,” said Constantine Cannon partner Matthew Cantor, who represents the plaintiffs. “Other hospitals were able to provide the same services that Sutter did without resorting to restrictive contracting practices.”
The case centers on Sutter Health’s “all-or-nothing” contracts with five major California health insurers — Anthem Blue Cross, Blue Shield, Aetna, Health Net and United Healthcare.
With 24 hospitals, 36 surgery centers and 12,000 doctors, Sutter has been described as an 800-pound gorilla in Northern California.
Cantor said Sutter Health took advantage of that market power to coerce insurers into buying its hospital services in San Francisco, Sacramento, Santa Rosa and Modesto, where there was more competition from providers like Dignity Health and UCSF, because the insurers really wanted to include its hospitals in Antioch, Auburn, Crescent City, Davis, Jackson, Lakeport and Tracy, where Sutter was the only option.
Cantor said these all-or-nothing contracts were effectively illegal tying arrangements.
“Again and again Sutter was able to force the health plans into contracts they did not want,” Cantor said.
He said Sutter also prevented health insurers from steering consumers toward cheaper care providers, or using tiered plans as an incentive for patients to go elsewhere. Sutter conditioned its participation in a tiered plan on being placed in the most favorable tier, thus making these products untenable.
Health insurers were also forced to pay Sutter’s “non-participating rate,” which was 95% of a patient’s billed charges, if they decide to keep Sutter’s hospitals out of network.
The lead plaintiffs — a handful of individuals and two small businesses — claim these practices caused 3 million California families and businesses to collectively pay nearly $411 million in insurance premium overcharges between 2011 and 2017.
Sutter’s attorneys pointed the finger at the health insurers for burdening consumers with higher premiums.
"Insurance company witness, they were not unbiased. Let's be serious,” said Jones Day partner Jeffrey LeVee “The insurance company witnesses had a lot of money at stake in this trial. They may not be the plaintiffs in name, but they were the true plaintiffs in this case and that was apparent in the advocacy with which they spoke.”
LeVee said the health plans had the option not to contract with Sutter but in reality, they all really wanted Sutter’s hospitals.
“Every insurer testified that they want broad networks that include all Sutter hospitals. Whether they did it in 24 separate contracts or with one agreement, they were already going to contract with every one. Systemwide contracts do not create a tie,” he said.
On the subject of tiered and narrow networks, David Kiernan, also a Jones Day partner, said these products benefit health plans, but lead to surprise bills for consumers. “They call it freedom but what they really want is control. Insurance companies want to pay less for our healthcare.”
Kiernan said Sutter “fought back” against tiered and narrow network products because they “didn’t want patients to slip through the cracks.”
“Doing something that's right for people is not an antitrust violation,” he said.
Cantor said Sutter had not offered any statistics on how often surprise billing occurs.
“We all know it happens, but does that warrant narrow and tiered products to not be offered at all? Of course not. Because at the end of the day the marketplace should make the decision as to what products get on the market and what products should succeed, not Sutter,” Cantor said. “This isn't a centrally planned economy. Sutter is not an autocrat.”
The case marks the first antitrust class action against the giant hospital network to go before a federal jury and has nationwide implications for how hospitals contract with insurers.
Plaintiffs are asking for $411 million in damages, but the federal judge overseeing the case has the discretion to triple that amount to $1.2 billion.
Cantor made a point of noting that the requested relief is less than the amount Sutter pays its top 25 executives. Though U.S. Magistrate Judge Laurel Beeler limited how much the jury could hear about executive compensation in the trial, Cantor was able to show that Sutter paid its "C-suite" level officers $453 million in salaries, benefits and other perks from 2009-2019.
While Sutter has argued that its hospitals are not higher-priced, an internal email from former Chief Financial Robert Reed revealed the contrary.
"Our current business model is dependent on commercial insurance. We are really more expensive than community average,” he wrote to Sutter’s then-CEO Chris Fry. “Therefore our current business model is reliant upon pooling our more expensive product offering with lower cost non-Sutter providers in an insurance wrapper to achieve a competitive average.”
Cantor described this email as a nail in the coffin moment for Sutter.
“If Sutter was so reasonably priced and of such high quality, why would the provisions in these contracts be necessary?” he asked the jury. “Sutter’s case doesn't add up. It knew it was high-priced and that it offered average quality, and without these clauses it had to compete on price and it couldn't do that. Sutter kept prices high through anti-competitive means. This was unjust and illegal.”
Subscribe to Closing Arguments
Sign up for new weekly newsletter Closing Arguments to get the latest about ongoing trials, major litigation and hot cases and rulings in courthouses around the U.S. and the world.