A new CDC report models how the new strain and existing ones will spread over the next several months, showing explosive numbers without widespread vaccination.
(CN) — Having dominated England for the last month, a new, more transmissible strain of coronavirus is expected to do the same in the U.S. by March, the Centers for Disease Control and Prevention reported Friday.
The U.K. strain, first reported on Dec. 14, has already become the dominant variant circulating in England. It has now shown up in 30 countries; the U.S. has seen 76 cases across 10 states, according to CDC data from Jan. 13.
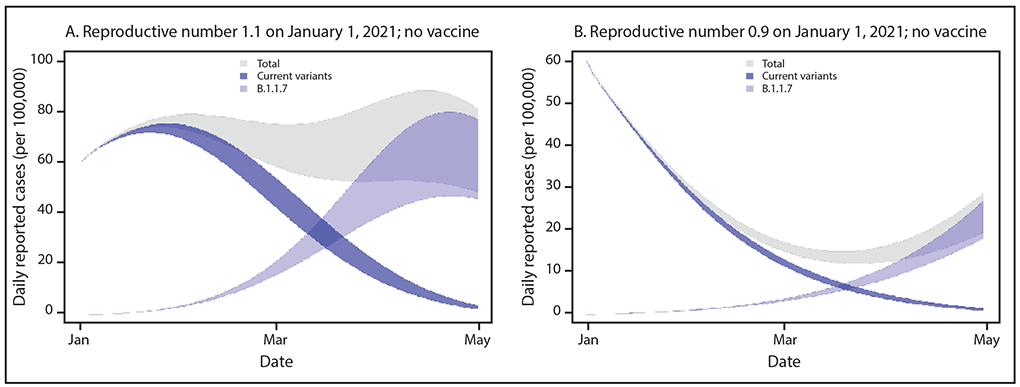
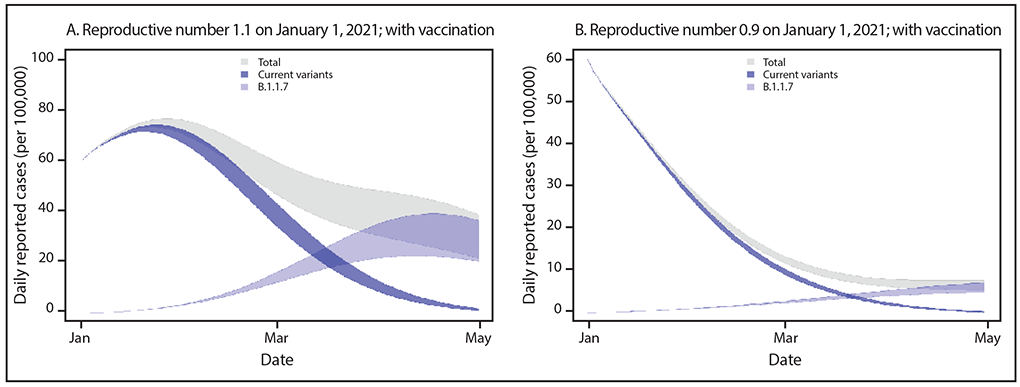
In the new CDC report, researchers present models for how efficiently the new strain, B.1.1.7, is spread, compared with three previously known variants of the coronavirus, officially called SARS-CoV-2.
Precisely how prevalent the U.K. strain is in the States is unclear, but it’s on track to take over.
“The modeled trajectory of this variant in the U.S. exhibits rapid growth in early 2021, becoming the predominant variant in March,” researchers wrote in the report, released Friday.
So far, there don’t seem to be clear differences in symptoms of patients infected with the new strain, compared to the virus the world has been battling for nearly a year.
Urging caution, however, the CDC warns that increased transmission could make more people sick, straining health care resources and crowding hospitals already nearing capacity. It also means the bar may be higher for herd immunity, often hailed as the proximate “end” of the pandemic.
Fighting against the new strain means, in part, extending vaccine distribution to more populations, the CDC report says. The vaccines being used in the U.S., created by Pfizer and Moderna, have both been touted by the companies as also protecting against the U.K. variant.
Even more important, for the time being, is that people continue wearing masks, physically distancing, frequently washing their hands and, when necessary, quarantining or isolating.

Dr. Benjamin Linas, an associate professor of epidemiology at Boston University School of Medicine, pointed to models showing that more effective transmission decreases are the result of measures besides the vaccine itself.
“At this time, it’s the non-pharmacologic interventions — masks, distancing, all the things that we’ve been doing — that really have been holding up the house, and are going to continue to do so,” Dr. Linas said Wednesday, speaking on a panel of experts discussing vaccine rollout. “We can’t rely on vaccine yet to be our protection.”
In the United States, vaccine distribution has been delegated entirely to state governments, each devising their own plans for administering shots. Multiple health departments officials and medical experts have called for greater federal guidance on that front.
“We can’t forget: pandemics, viruses, do not respect state borders,” said Dr. Bob Hopkins, a professor at the University of Arkansas for Medical Sciences. “What’s happening in Arkansas is happening in Tennessee.”
Hopkins also chairs the National Vaccine Advisory Committee of the U.S. Department of Health & Human Services. He spoke on the same panel as Dr. Linas, who agreed that a decentralized rollout has not benefited the U.S.
“You can’t respond to a global pandemic, which is absolutely a national priority, with piecemeal, state-by-state responses,” Dr. Linas said.
“We’re finding over and over again that the rights-based individualistic approach, to what’s inherently a communal problem, doesn’t work,” he continued. “It’s bankrupt. It has no response to this crisis.”
As of Friday, 31,161,075 doses of vaccine have been given out, according to CDC data — although there is a lag between when doses are administered and when they’re actually reported to the database.
The CDC, along with its academic and institutional partners, is continuing to sequence genetic material from viruses to identify new variants — and trace the ones we already know about, some of which are poised to make the pandemic even worse.
Viruses survive by rapidly mutating, which helps them find new homes in the cells of animals. Not every variant of the coronavirus that causes Covid-19 will become dominant; “some mutations in the viral genome emerge and then recede,” the CDC report notes.
But mutations that give a virus variant a selective advantage — like higher transmissibility — are likely to take hold.
In the case of the UK strain and others, the competitive edge comes from a mutation that changes how the virus binds to cells by modifying what’s called a spike protein, or S protein. The protein is essential for a virus to make its way into a host and helps to facilitate its spread.
Coronavirus variants with spike protein mutations have appeared in parts of the globe other than the U.K., the CDC reports. In late fall 2020, one such strain was detected in South Africa; another was seen in travelers from Brazil during routine screening at an airport in Tokyo.
“These variants carry a constellation of genetic mutations,” the CDC report states. The two variants may not only increase transmissibility, but also reduce how susceptible the virus is to being neutralized by antibodies.
So far, neither strain has been found in the U.S.
Subscribe to our free newsletters
Our weekly newsletter Closing Arguments offers the latest about ongoing trials, major litigation and rulings in courthouses around the U.S. and the world, while the monthly Under the Lights dishes the legal dirt from Hollywood, sports, Big Tech and the arts.

 Search Articles
Search Articles